Shouldn’t Everyone Be Treated The Same? The Pursuit of Fair Access to Health Care
The World Health Organisation is campaigning for “Building a fairer, healthier world” in 2021.
Subscribe to our Telegram channel for the latest stories and updates.
Never mind the family you were born into, just the mere fact of your birth place, your quality of life could vary significantly. For example, one of the things that determine your quality of life is health care.
Access to health care has come a long way in the last century but it still has a long way to go before everyone is afforded the basic necessities health care provides.
The gap between who gets it and who doesn’t needs a concerted effort on a global scale to be decreased and this unequal access to health care is known as a health inequity.

What is World Health Day ?
This 7th April 2021 is World Health Day and The World Health Organisation (WHO) is calling for action to eliminate health inequities as part of a year-long global campaign to bring people together to build a fairer, healthier world.
The enjoyment of the highest attainable standard of health is one of the fundamental rights of every human being without distinction of race, religion, political belief, economic or social condition.
World Health Organisation constitutional principle.

Who ever said the world was fair ?
Renowned for the affordable access to healthcare are places like Canada, UK, and many of the European countries. These places prioritise the health of their people rather than commodifying people’s health, and such practises should be adopted on a global scale.
In recent years many countries have experienced rapid economic growth, migration and urbanisation; creating opportunities for better lives for many, but leaving others behind.
Yet, all over the world, some groups struggle to make ends meet with little daily income, have poorer housing conditions and education, fewer employment opportunities, experience greater gender inequality, and have little or no access to safe environments, clean water and air, food security and health services. This leads to unnecessary suffering, avoidable illness, and premature death. And it harms our societies and economies.
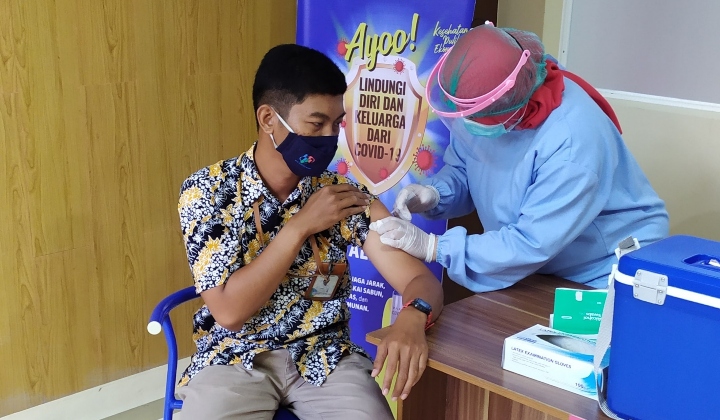
Healthcare in Malaysia
The Malaysian healthcare system focuses on Primary Health Care (PHC) that places social equity as important and allocates public funds for the poorest 20% of the population.
After independence, the health sector became an integral part of the national and development process and the Ministry of Health (MOH) has been able to deliver health care to communities throughout the country.

Studies have also shown that the Malaysian health standard is almost at par with those of developed countries. Malaysia ranked fairly high for our healthcare in the region, and in fact – the world. Data from the World Health Report indicated that the health indicators of Malaysians were much better compared to some of the ASEAN countries. As a nation, this puts us in a good position to help our neighbours improve their healthcare systems.
But is Malaysian health care equitable?
Despite its quality, the Malaysian healthcare system is not without its flaws.
A 2011 paper published in the Journal of Public Health Africa pointed out that despite Malaysia’s effort in socio-economic development plans, there still exist issues in equity and accessibility especially for the indigenous groups, rural population and the hard-core poor. This can be seen through quality in terms of health services, manpower and equity in terms of geographical location and accessibility in terms of price and tariff.
Nevertheless, efforts are taken by the government to strengthen the rural health services in Malaysia through the improvement of existing facilities and introducing new health services that range from outpatient curative care to preventive and promotive services.
Health care delivery in Malaysia: changes, challenges and champions, Journal of Public Health Africa

(Credit: Effendi Abdulgani/YouTube)
The paper also noted that the difference in Malaysia’s public and private health sectors in terms of specific services provided may have a significant effect on the equity of services. It also leads to an imbalance of the distribution of manpower between the public and private sectors here in Malaysia.
Generally, the services provided by private hospitals are curative and selective in nature, either free or subsidized and much more comprehensive which is controlled by issues of equity. Access to private health services is limited to the richer society that can afford out-of-pocket payments of higher fees.
Health care delivery in Malaysia: changes, challenges and champions, Journal of Public Health Africa

(Credit: The Star)
Unfair & Preventable Health Inequity
The Covid-19 pandemic has undercut recent health gains, pushed more people into poverty and food insecurity, and social and health inequities.
Covid-19 has hit all countries hard, but its impact has been harshest on those communities which were already vulnerable, who are more exposed to the disease, less likely to have access to quality healthcare services and more likely to experience adverse consequences.

Health inequities are not only unjust and unfair, they are preventable. They threaten the advances made to date, and have the potential to widen rather than narrow equity gaps.
Doesn’t mean we can’t make the world fairer
In the case of the vaccine for the Covid-19 pandemic for instance, by prioritising front-liners, the elderly and the sick, instead of the wealthy, powerful, and famous; we can demonstrate that the world doesn’t have to be so unfair all the time. That human lives matter more than the privileges we are born into.
How can we systematically support access to health care in impoverished nations? The first step to solving a problem is recognising that there is one. Many countries in Africa and South America, even regionally in our back yard, Southeast Asia, require international assistance to upgrade their quality of health care for their people.
Strategies that place greater attention to improving health equity, especially for the most vulnerable and marginalised groups can alleviate these inequities.

Equitable Access
During 2020, as the Covid‑19 pandemic escalated globally and vaccine development intensified, the WHO Covid-19 Vaccines Global Access (COVAX) facility adopted the motto “No one is safe unless everyone is safe” to emphasise the need for equitable vaccination.
The facility set a goal of supplying vaccines to nearly 100 low-to-middle income countries that could not afford them. COVAX sought to fundraise US$6.8 billion to purchase and deliver vaccines to these participating countries.
WHO is calling on leaders to ensure that everyone has living and working conditions that are conducive to good health, and to monitor health inequities and ensure that all people are able to access quality health services when and where they need them.
As they once sang “Heal the world, make it a better place, for you and for me and the entire human race.”
Share your thoughts with us on TRP’s Facebook, Twitter, and Instagram





